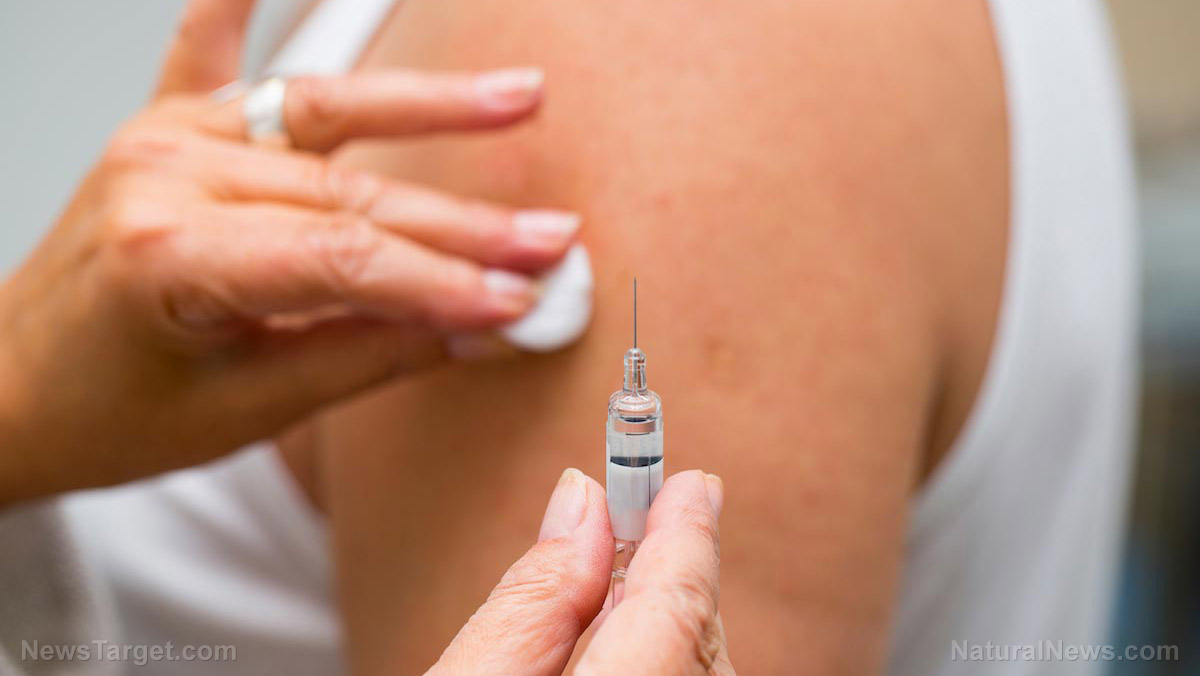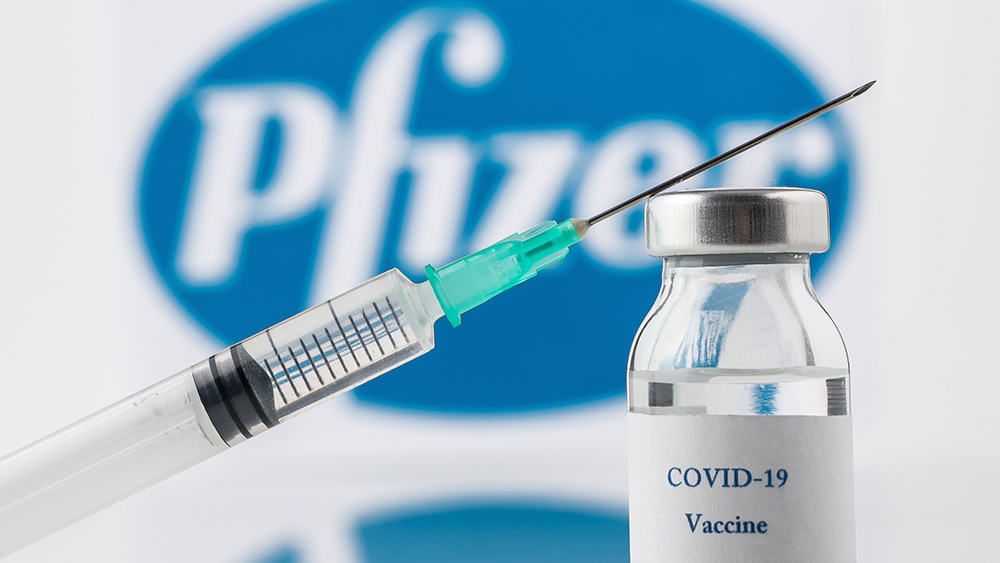
As new infections and breakthrough cases continue to rise across the globe, it is fast becoming clear that the Wuhan coronavirus (COVID-19) vaccine experiment is a massive failure.
Israel is perhaps the biggest proof of that. The country has one of the fastest vaccine rollouts in the world. Nearly 80 percent of eligible Israelis ages 12 and above have been vaccinated. Approximately 2.35 million Israelis have also received booster doses.
Yet, new data from the University of Oxford reveals that Israel has the highest number of COVID-19 cases per capita.
On Sept. 3, Israel had a rolling seven-day average of 1,143 COVID-19 cases per million people – more than double the rate reported in the U.S. on the same day, which is 501 per million.
The Jerusalem Post recently reported that since the beginning of August, nearly 200,000 Israelis have tested positive for COVID-19 and 564 people have died with a COVID-19 diagnosis. In early August, Israel's Ministry of Health reported that 64 percent of the country's 400 COVID-19 patients in serious condition were fully vaccinated.
It's not really surprising as Israel's preliminary vaccine data published in July found that Pfizer's COVID-19 vaccine was just 40.5 percent effective on average at preventing symptomatic infections. (Related: All of the evidence is in: The covid vaccine is a failure.)
The analysis, which was carried out as the delta variant became the dominant strain in the country, appeared to show a waning effectiveness of the Pfizer vaccine. It was only 16 percent effective against symptomatic infections for those who had two doses back in January. For people that had received two doses by April, the efficacy rate against symptomatic infection stood at 79 percent.
Vaccine does nothing to reduce COVID-19 transmission
In a recent article published by the Wall Street Journal, neurologist Dr. Michael Segal explained why people vaccinated against COVID-19 are still contracting and spreading the disease at a high rate.
Segal wrote that the vaccines only stimulate internal immunity but do nothing to address mucosal immunity. Internal immunity protects the inside of the body while mucosal immunity provides the first line of defense by protecting the nose and mouth, and by doing so also reduces spread to others.
He said that all COVID-19 vaccines "are largely ineffective at stimulating the secretion of a particular form of antibodies called Immunoglobulin A (IgA) into our noses that occurs after actual infection with a virus."
Meanwhile, those who have contracted and recovered from the disease have both mucosal and internal immunity. They have what they call a natural immunity from the disease.
That's the reason why some experts are now recommending that the virus be allowed to circulate throughout the population, with precautions taken for vulnerable individuals.
"We really cannot do anything else but allow the virus to take its course in order for the population to achieve herd immunity," said Porolfur Gudnason, chief epidemiologist of Iceland's Directorate of Health. "We need to try to vaccinate and better protect those who are vulnerable but let us tolerate the infection. It is not a priority now to vaccinate everyone with the third dose."
Some are asking whether catching COVID-19 now is better than more vaccines. (Related: COVID-19 natural immunity vs vaccine-induced immunity guide.)
"If you had a real humdinger of an infection, you may have better immunity to any new variants that pop up as you have immunity to more than just spike [protein]," said Eleanor Riley, an immunologist from the University of Edinburgh. "We could be digging ourselves into a hole, for a very long time, where we think we can only keep COVID away by boosting every year."
Recovered COVID-19 patients retain broad and durable immunity
Multiple studies found that most people who have recovered from COVID-19 retain a broad and durable immunity to the disease.
After people recover from infection with a virus, the immune system retains a memory of it. Immune cells and proteins that circulate in the body can recognize and kill the pathogen if it's encountered again, protecting against disease and reducing illness severity.
An Emory University study published in the journal Cell Reports Medicine found that most of the patients who recovered mounted a strong and wide-ranging immune response to the virus for at least the 250-day duration of the study.
The study involved 254 COVID-19 patients between 18 to 82 years old, who provided blood samples at various points for a period of over eight months beginning April last year. About 71 percent of the patients had mild disease, 24 percent experienced moderate illness and five percent had severe disease.
Another study, which was published on Jan. 6 in Science, analyzed immune cells and antibodies from almost 200 people who had been exposed to SARS-CoV-2 and recovered.
Antibodies against the spike protein of SARS-CoV-2 were found in 98 percent of participants one month after symptom onset. The number of antibodies ranged widely between individuals, but their levels remained fairly stable over time, declining only modestly at six to eight months after infection.
Follow Immunization.news for more news and information related to coronavirus vaccines.
Sources include:
Please contact us for more information.