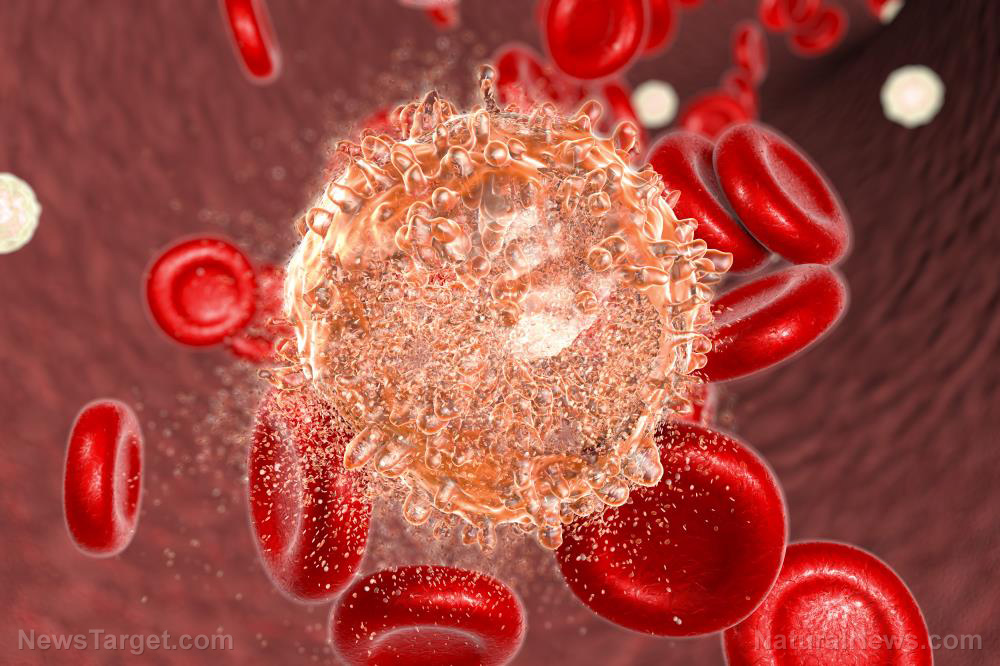
British pharmaceutical firm GSK announced that it will stop selling its blood cancer drug Blenrep in the United States.
The company announced on Nov. 22 that it has begun the process to withdraw the drug's marketing authorization in the country. It clarified, however, that trials for the drug would continue and that some patients would be given the option to enroll themselves for continued access to the treatment.
"We will continue the Driving Excellence in Approaches to Multiple Myeloma (DREAMM) clinical trial program and work with the U.S. Food and Drug Administration (FDA) on a path forward for this important treatment option for patients with multiple myeloma," GSK Chief Medical Officer Dr. Sabine Luik said in a statement.
The FDA speedily approved Blenrep in the U.S. in 2020, permitting its use for patients with relapsed or refractory multiple myeloma who received at least four previous therapies. In 2021, total worldwide sales for the drug reached £89 million ($105.78 million) – with U.S. sales comprising two-thirds of this amount.
Despite its impending withdrawal in the U.S. market, a GSK official told Reuters that Blenrep continues to be marketed in the 17 countries where it has been approved. Most of these countries are in the European Union, where the company is still discussing the latest clinical data about the drug with the bloc's health authorities.
According to Reuters, "Blenrep belongs to a category of treatments called antibody-drug conjugates, which are engineered antibodies that bind to tumor cells and then release cell-killing chemicals."
The company explained that the withdrawal stemmed from Blenrep failing the main goal of a key study. The said trial sought to prove that the blood cancer drug was better than an existing drug on the market. Blenrep's failure raised doubts about its future in the U.S. market, given the FDA's potential withdrawal of its marketing authorization. (Related: Yet another vaccine failure: Widely-hyped GSK cancer vaccine fails in clinical trials.)
GSK's earlier ovarian cancer drug suffered a similar fate
The failure of GSK's multiple myeloma treatment was another setback for the company's oncology business, which it deems a key area of focus. GSK was earlier forced to limit the use of Zejula, its treatment for ovarian cancers, as a second option.
Zejula falls under a family of drugs called PARP inhibitors that block the release of the eponymous enzyme poly ADP ribose polymerase (PARP). Cancer cells make use of this protein to repair themselves and grow, and treatment with Zejula ensures that cancer cells are killed off.
However, PARP inhibitors have been plagued by safety setbacks – leading to restrictions on Zejula. In September, GSK withdrew the use of the drug in certain ovarian cancer patients who had previously undergone three or more chemotherapy regimens. This restriction stemmed from clinical trial data that suggested patients treated with Zejula do not live as long as those given other drugs.
Reports later emerged that FDA advisors were set to review Zejula's use in a second-line setting, that is as a therapy designed to keep cancer at bay for those with recurring cancers, following additional data from a key study. GSK confirmed that it had complied with the regulator's request to restrict the use of Zejula.
The PARP inhibitor was not developed by the British drug maker. Rather, it was acquired through GSK's 2018 purchase of the Waltham, Massachusetts-based Tesaro – to the tune of $5.1 billion.
According to Reuters, Zejula racked up a total of £120 million ($142.62 million) in worldwide sales for the third quarter of 2022. A GSK spokesperson added that about a quarter of the drug's U.S. sales were from the second-line indication. They added that Zejula's second-line indication outside the U.S. has no changes.
Head over to BigPharmaNews.com for more stories about cancer drugs and drug manufacturers.
Watch Health Ranger Mike Adams recounts a woman curing her blood cancer by taking curcumin from turmeric, instead of dangerous drugs like Blenrep.
This video is from the Health Ranger Report channel on Brighteon.com.
More related stories:
Most cancer drugs make it to the market without any proof they're safe or effective.
Breast cancer drug lapatinib ACCELERATES cancer cell growth, concludes new study.
Big Pharma conspired to destroy supply of life-saving cancer drugs by putting profit before people.
Sources include:
Please contact us for more information.













