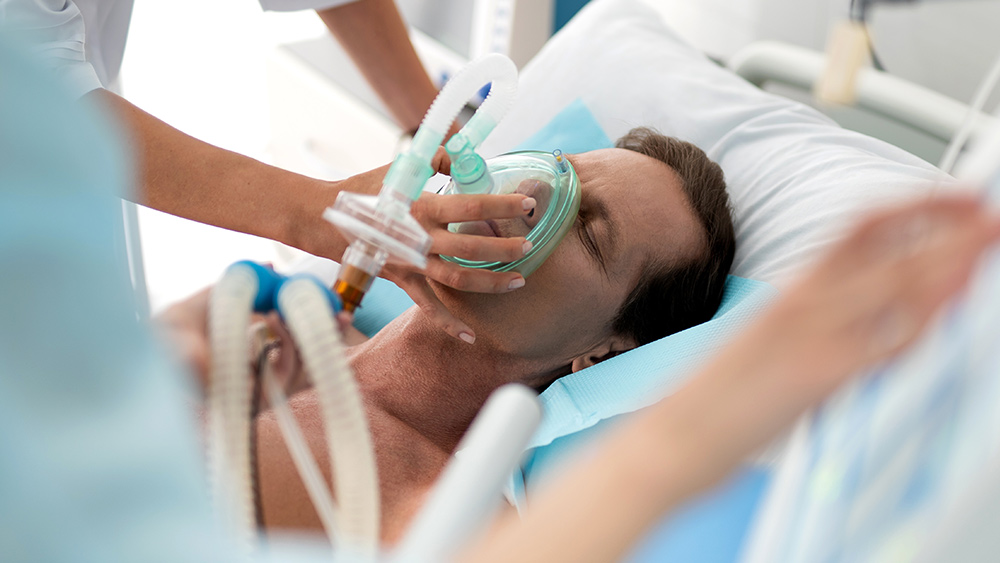
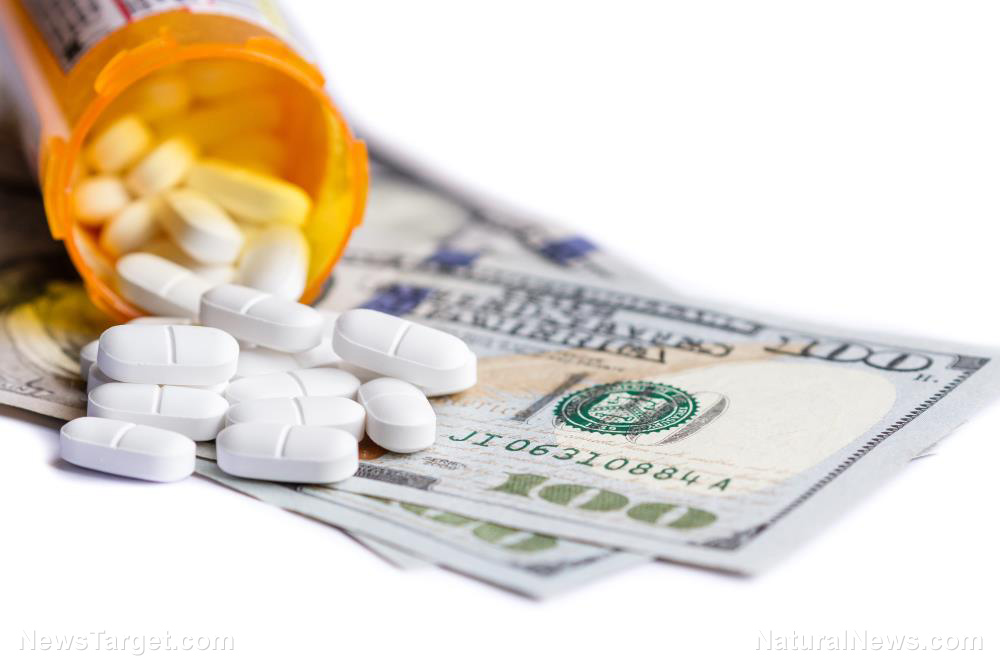
Some of the medical professionals who have been taking advantage of their patients and manipulating healthcare benefits for financial gain are finally being held accountable thanks to the largest healthcare fraud and opioid takedown enforcement action in DOJ history.
Yesterday, law enforcement officials announced the historic roundup. A total of 345 defendants were charged across 51 federal districts; more than 100 doctors, nurses and other medical professionals were among those charged.
The defendants are being charged with submitting over $6 billion in fraudulent claims to private insurance and federal healthcare programs. This includes more than $845 million related to substance abuse treatment facilities, over $806 million in connection with illegal opioid distribution schemes and other healthcare fraud, and $4.5 billion related to telemedicine.
Some of the agencies involved in the takedown included U.S. Attorney’s Offices, the FBI, DEA and HHS. It is part of an ongoing effort to crack down on the devastation caused by the opioid epidemic and related healthcare fraud.
The action sheds light on the role that doctors and other healthcare professionals have been playing in the nation's deadly opioid epidemic. DEA Assistant Administrator Tim McDermott said: “The opioid epidemic our country is battling is exacerbated when unscrupulous individuals seek to profit from people, in particular those confronting addiction.”
“When doctors, pharmacists, and individuals exploit the weakness of a fellow human being in order to line their own pockets, DEA will use every tool at its disposal to stop and bring them to justice,” he added.
They announced cases of illegally prescribing and distributing opioids involving more than 240 defendants who submitted more than $800 million in false claims to Medicare, Tricare, Medicaid and private insurance for treatments that were medically unnecessary and often were never even provided to the patients.
Kickbacks and bribes for treatments patients never received
The agencies explained how patient recruiters and other co-conspirators received cash kickbacks for giving providers beneficiary information, which they then used to submit fraudulent bills to Medicare. In addition, some medical professionals were charged for the distribution of more than 30 million doses of prescription narcotics such as opioids.
Telemedicine fraud made up the bulk of the fraud, with more than $4.5 billion in fraudulent claims relating to telemedicine schemes. In many cases, telemedicine executives were charged with paying doctors and nurses to order durable medical equipment, testing and medications the patients did not need without interacting with them at all or after brief telephone conversations. Companies providing durable medical equipment and genetic testing, along with pharmacies, then purchased these orders in exchange for bribes and kickbacks and sent false claims to Medicare for them. A total of 256 medical professionals lost their Medicare billing privileges on account of their involvement in such schemes.
The ”sober homes” cases included charges related to more than $845 million in fraudulent claims for tests and treatments given to vulnerable patients who were seeking treatment for alcohol or drug addiction. Doctors, substance abuse treatment facility owners and patient recruiters were alleged to have participated in schemes that saw illegal kickbacks being given for referring patients to these facilities and subjecting them to medically unnecessary drug testing and therapy sessions that were never provided.
Acting Assistant Attorney General Brian C. Rabbitt said: “The cooperative law enforcement actions announced today send a clear deterrent message and should leave no doubt about the department’s ongoing commitment to ensuring the safety of patients and the integrity of health care benefit programs, even amid a national health emergency.”
It is good news for our country to see the authorities coming down hard on those who take advantage of vulnerable people and contribute to the deadly opioid epidemic that is costing so many American lives, not to mention taxpayer dollars.
Sources for this article include:
Please contact us for more information.